'Social distancing, wearing masks and hygiene should be practised more strictly.'
'People should not assemble in close spaces as the micro droplets may hang in the air and can last for a longer time.'

IMAGE: Recovered patients at the CWG Village COVID care centre near Akshardham in New Delhi, July 23, 2020. Photograph: Kamal Kishore/PTI Photo
From the scientific community to the medical community to the community as a whole, every adult on this planet is perplexed, nervous and scared about the coronavirus.
Life in the times of the coronavirus is not the same as it was before it surfaced in Wuhan, China, and thereafter spread to every part of the planet. This is the new normal.
Scientists and medical professionals are learning new things about the virus every day.
Shobha Warrier/Rediff.com speaks to doctors and scientists about their experiences combating the coronavirus.
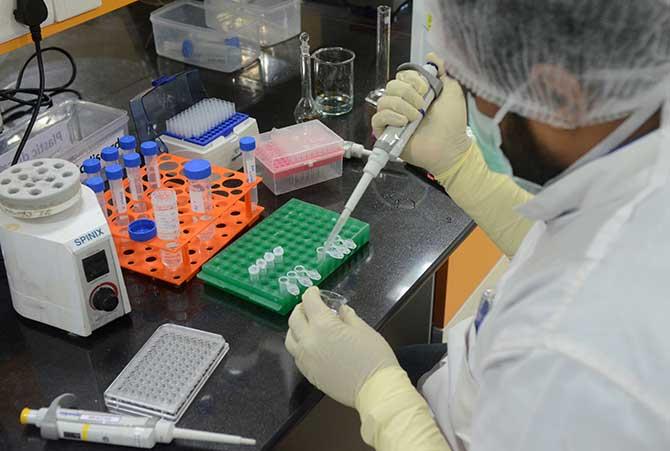
IMAGE: A laboratory at the Serum Institute of India, the world's largest maker of vaccines, which is working on vaccines against the coronavirus. Photograph: Euan Rocha/Reuters
Dr Rakesh Mishra, Director, Centre for Cellular and Molecular Biology in Hyderabad, and his team discovered a new strain of the novel coronavirus, Clade A3i.
The CCMB scientists found that A3i came not from China or Europe, but from South East Asia and this strain is responsible for around 41% of the cases in India.
Dr Mishra lists what he has learnt about the coronavirus:
- We have observed that the virus is mutating not so fast and, as a result, the major clade all over the world remains to be a common one, which is A2a.
The other major clade which is unique to South East Asia, A3i seems to be disappearing gradually.
This is an encouraging trend for those who are developing the drugs and vaccines.
- There have been several reports including our own initial efforts, that found the virus can be detected in river bodies near the infected population or the sewage system in the cities, and this would give an indication of the infection load in the catchment areas.
This knowledge would be very useful for the current as well as the future surveillance and monitoring of infectious diseases like COVID-19.
- Recent studies have shown that COVID-19 can also be present in small droplets, <5 micron size, which does not necessarily mean that the virus is airborne.
However, this means that the virus can stay in the areas for a much longer time than the bigger droplets, as was had thought earlier.
This means that social distancing, wearing masks and hygiene should be practised more strictly.
People should not assemble in close spaces as the micro droplets may hang in the air and can last for a longer time in such situations.

IMAGE: Medics undergo a mock-drill to treat COVID-19 patients. Photograph: PTI Photo
Dr Himanshu Reddy Dandu of the King George's Medical University in Lucknow led a team treating coronavirus patients.
In the last three months, Dr Dandu says, the doctors treating covid patients have learnt a lot.
- In March, when we first started treating covid patients, it was all about keeping all the sick people on ventilators.
As days pass by, we learnt that it was not necessary to put them all on ventilators, instead we need to only give them oxygen and make them rest.
We understood that what we had to do was to maintain the oxygen level as much as possible so that the lung recovered slowly.
This is the major learning we had on the treatment part of the infection.
- We also understood now that most of the patients, that is 80% to 85% are asymptomatic or very mild symptomatic.
When we spoke in March, though we knew that the mortality rate would be low, we thought all the covid patients would develop fever, breathlessness, etc.
Now, we know that many of them do not have any fever; some develop mild diarrhoea or loss of smell, and most of them do not have any symptoms at all.
The guideline initially was to test anyone with fever and sore throat, but now we understand that people may not have any of the symptoms, and still will have the coronavirus.
- Initially, there was some doubt about people developing antibodies and herd immunity.
Now, I personally feel that people will develop herd immunity.
For example, if you look at the countries which were severely affected in March and April, they have opened up now, like Spain, South Korea, Japan, Italy, etc.
Even after opening up, the cases have not gone up exponentially, and it is under control.
This shows these countries have developed herd immunity.
If there was no herd immunity, cases would have gone up.
So, looking at the epidemiology of the countries that are infected, we see that they have developed herd immunity.
But how long this immunity will sustain, only time will tell.
It is now learnt that the antibodies will work only for 3 to 4 months.
Generally, viral immunity is based on T-cells, or the memory cells but we are not sure about the coronavirus patients developing memory cells yet.

IMAGE: A worker from the Bharatiya Jain Sanghatana, a non-governmental organisation, wearing a 'Smart Helmet', a portable thermoscanner that can measure the temperature of people at a distance, screens residents in a slum in Mumbai, July 23, 2020. Photograph: Hemanshi Kamani/Reuters
Dr Vaibhav Agavane, an epidemiologist who is currently a faculty member at the Institute of Public Health, Bengaluru, told me in March that even asymptomatic patents can spread the coronavirus.
He lists what he has learnt about COVID-19:
- Asymptomatic cases - A high proportion (approximately 40% to 45%) of the people who are infected with the SARS-CoV-2 are likely to have no symptoms.
For majority of the population which will contract the infection, it is going to be an asymptomatic infection or mild viral disease.
- Infectivity during pre-symptomatic phase: This fact has wider implication in our ability to control the pandemic.
Those who get infected can infect others irrespective of whether they develop or not develop the symptoms.
Thus, it is particularly important that we immediately isolate the identified cases and quarantine the contacts to further decrease the transmission.
Getting this done is an uphill task but it is very important.
- Secondary attack rate: The secondary attack rate is the proportion of household members of COVID-19 patients who develop the disease because they stay with them.
This rate for SARS-CoV-2 is higher than that of the other viruses like SARS-CoV to which it is closely related.
Overall, it is highly transmissible from one person to another.
The good news is that taking preventive steps like the use of masks, protection of the eyes, keeping physical distance of preferably 2 metres, practicing hand hygiene are likely to decrease the probability of getting infected even in such a scenario.
Feature Presentation: Ashish Narsale/Rediff.com
















