'Call it by whichever name, but there is transmission happening between people.'
Ruchika Chitravanshi reports.
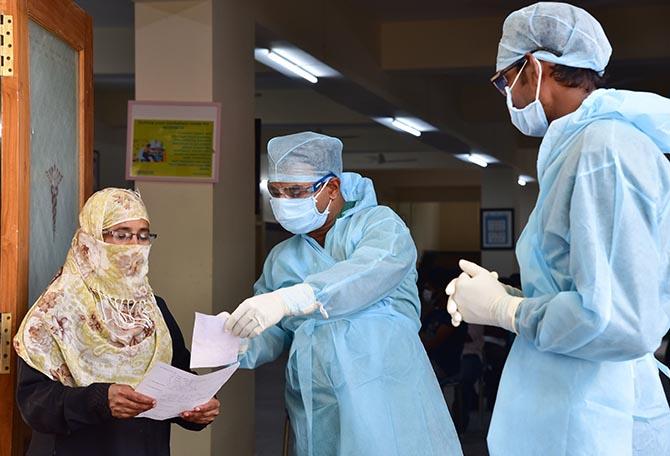
A few days ago, a woman in her sixties reached a hospital in Dwarka, New Delhi, with fever, cough and breathing difficulty. The scans showed her lungs were completely clouded in white. It was a textbook case of coronavirus.
The information provided by her family, however, did not indicate any foreign travel or link to a traveller till her son decided to share he had recently been to Thailand.
"People are often not forthcoming with information fearing taboo associated with Covid-19 patients," said Sharang Sachdev, who heads the emergency division at the Aakash Healthcare in Dwarka.
Not all cases are as straightforward. Over the last two weeks, there has been a rise in the number of cases with no contact history to justify their infection.
Even as the government races to trace contacts of COVID-19 patients, officials have continued to ward away any suggestion of community transmission.
Against that backdrop, confirmed cases among health workers, nurses and doctors have sent the alarm bells ringing.
A recent random sampling of patients of severe acute respiratory infection found several confirmed positive cases with no foreign travel history or contact with any infected person.
'These cases need to be investigated further... If there is community transmission, we will be the first to come and tell you as we would want everyone to be more alert,' said Lav Agarwal, joint secretary of the health ministry, at a press briefing on COVID-19.
But the question keeps coming back. Is India in community transmission?
As the country continues on the upward trajectory in the fourth week of nationwide lockdown, epidemiologists feel it is a matter of semantics.
"If the contact of a contact gets infected, the virus has infiltrated the community. In my definition, community transmission is here... The government is denying it out of conviction and not lack of transparency," said Dr Jacob John, virologist and former chief of the Indian Council of Medical Research.
"I would say they are not looking wide enough. The absence of evidence is not evidence of absence of community transmission," Dr Jacob said.
The strategy adopted in India consists of five stages of which we are currently in the third -- large outbreak amenable to containment.
Community transmission comes next, followed by endemic.
"If you are not doing enough testing and you don't know where the doctors are getting infected from, maybe there's community transmission going on. I think it's safe to say that you should maybe start acting as if there is community transmission even if it has not started," said DR Maxwell Salvatore, biostatistics researcher, Michigan University.
While that is true, questions have been raised about India's testing strategy which has remained the same even in the face of looming community transmission.
"You have already taken the hardest measure on social distancing. What you really need to work on is testing in high contact and high density areas so that you can easily track the pulse of the epidemic," said Dr Bhramar Mukherjee, professor of epidemiology, University of Michigan.
Hospitals not willing to risk health workers and other patients have already started testing all patients who are showing up at their emergency wards.
At Max hospital, for instance, high suspect cases and those with moderate symptoms are being given an individual test and for those who are non-symptomatic many hospitals are conducting pool tests, with five samples in one pool.
"There are many cases where we don't know the source of contact... Now even if we get a patient who tests negative for coronavirus but no other infection can be established, we treat it as COVID-19 and take those levels of precautions... Many times it takes more than a couple of tests to show a positive result," said Dr Sandeep Budhiraja, group medical director, Max Healthcare and senior director, Institute of Internal Medicine.
Dr Budhiraja also pointed at the rise in the number of pneumonia cases in April.
"Usually the peak of such cases is in January and February. By March, they dwindle and in April we hardly see such cases. This year it has been different," he said.
Experts say the strategy in India should change to a medicine-based approach over a public health-based testing.
"Medicinal response is based on evidence. You diagnose and treat. In public health, the goal is to protect the uninfected. You are finding evidence for transmission ... As an epidemiologist, I would say that is not right," Dr John said.
According to ICMR estimates, 69 per cent of COVID-19 infected were asymptomatic. The only way to trace such COVID-19 carriers was through extensive testing, according to experts.
India has conducted over 400,000 tests so far. Tests are in short supply and the strategy has been to rationalise their use.
The RT-PCR test to detect COVID-19 is only being given to symptomatic people with travel or contact history, patients of severe acute respiratory infection, healthcare workers who came in contact with COVID-19 patients and also asymptomatic contacts of a confirmed case and all patients with influenza like illness.
So, what would change if the government announces there is community transmission? The health ministry has said there will be a separate mitigation plan for community transmission and if India becomes endemic for COVID-19.
"If you acknowledge that, people will get a different message. Call it by whichever name, but there is transmission happening between people," Dr John added.