More vaccination would have been done in India if the State had not had complete control of all vaccination, notes Ajay Shah.
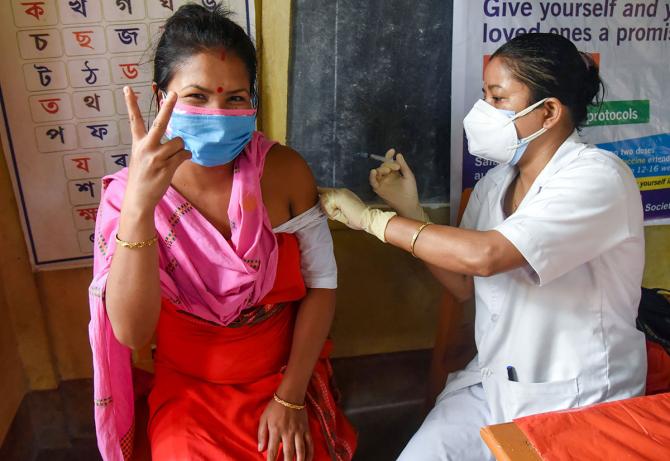
Something new has happened in Indian healthcare.
The State achieved the ability to apply coercive power and control every doctor-patient relationship in the context of COVID-19 vaccines.
Many flaws in India's COVID-19 vaccination story derive from this control.
Social outcomes are better, particularly in the Indian setting, when many people are thinking and responding.
We should be wary about the use of the coercive power of the State.
No two persons are alike. For each person, decisions about vaccination involve many considerations, including vulnerability to disease, lifestyle, and healthcare financing.
Some people in India get vaccines against the flu or against HPV, and these decisions are made in the privacy of the conversation between a doctor and a patient.
COVID-19 vaccination is no different. People who are less able to organise their life to be socially isolated require vaccines more.
People who live with the elderly require the vaccine more.
The choice of vaccine varies by person -- the AstraZeneca vaccine fares poorly with young women.
The precise history of the vaccination of each person shapes the optimal choices on boosters.
Ordinarily, the Indian health system features millions of decentralised decisions by healthcare providers and their patients.
Healthcare providers look at local conditions, and the information available at a point in time, and help each person make the best decisions.
Something new happened with the COVID-19 vaccine
The State achieved a new level of power.
It brought coercive power to bear on every doctor/patient relationship all over India.
Doctors and patients were disempowered, and all vaccination actions were controlled by the Union government.
Alongside this, State power was brought to bear on the pricing, import, export, and production of vaccines.
Many difficulties of COVID-19 vaccination in India derive from this strategy, of a Union government that has obtained complete control of every action regarding this.
The counterfactual that we should play in our minds is that of an Indian State that did nothing -- as is done with HPV.
In this case, by early 2021, many Indian organisations would have been importing vaccines.
Price signals would have elicited higher supplies from vaccine makers.
Thousands of healthcare organisations would have been doing a lot of vaccination.
Before the second wave, a larger number of people would have been vaccinated.
This would have helped through three pathways: Vaccinated people who don't die, vaccinated people who don't infect, and vaccinated people who don't load the healthcare system.
More vaccination would have been done in India through decentralised conversations between doctors and patients, when the emergence of the Omicron variant brought urgency to booster doses, if the State had not had complete control of all vaccination.
A wider range of vaccines would be in play if the State had not blocked imports, thus permitting better boosters to be deployed for each vaccinated person.

There is only one market failure in vaccines
The presence of a positive externality.
Each person that makes a decision to pay for a vaccine is inadequately concerned about the overall gains to society; the person will tend to underspend when buying a vaccine as she selfishly cares only about her own health and not the spillover benefits to others from her vaccination. There are three interesting facets to this market failure.
First, there is no harm to anyone when private people go to a private provider and get a vaccine.
Each vaccinated person is imposing a benefit upon society, of reducing opportunities for the virus to spread.
Second, the difficulties are only about the people who choose to not buy the vaccine.
Here, there can potentially be a role for the State in nudging these decisions by bearing part of the cost.
This is best done using vaccine vouchers. At most, governments can run tents or vans that dole out vaccinations, but there is no reason to interfere with others who are doing vaccination.
Third, for every person who makes the decision to buy a vaccine, the end outcome is the undistorted one.
Market failure influences the decision-making process of the person, but once the person decides to get the vaccine, the outcome is no different from one in which there was no market failure.
This is unlike the analysis of positive externalities in other fields -- eg, education -- where the purchase decision of every individual involves an underspend.
Underspend by buyers is the only market failure in the world of vaccines.
There is no other market failure, and thus no case for any other kind of State intervention.
It is unfair to evaluate the decisions of policymakers with the luxury of hindsight.
But there are principles in the field of public policy, which generated the right guidance all along.
Wisdom in public policy involves respecting the market process as the best path to organising the production side of the economy.
The price system would have resulted in better wholesale vaccine availability in India.
This involves not interfering with prices, production, imports, or exports. When the State starts controlling these aspects of the economy, this should make us uncomfortable.
Wisdom in public policy involves scepticism about grand schemes, about gigantism, and about state legibility (information in the hands of the government).
In the best of times, India is highly diverse and the Indian State has low capabilities.
In August and September 2020, it was not hard to see the limitations of a centrally planned vaccination programme.
Wisdom in public policy involves watching over every use of the coercive power of the State.
The Hippocratic oath of health policy should be: Above all, do no harm.
If a private person wants to push a vaccine into the arm of a person, this is only a good thing, and the State should not interfere.
When State violence is deployed to interfere in the outcomes of a doctor/patient conversation, this should make us uncomfortable.
Ajay Shah is an independent scholar.
Feature Presentation: Rajesh Alva/Rediff.com