
Do you know the risk of getting pregnant that each method of birth control involves?
Some kinds of birth control work better than others and different methods suit different people.
Here, we bring you a list of all possible precautions people use while having sex -- the higher the method comes on the list below, the better it works. The order is based on 'typical use', not 'perfect use'. Read on to learn more about different birth control methods.
Birth control methods in order of how well they work
Hardly any risk of getting pregnant: Failure rate under 1 percent
Implant
This is a tiny rod containing a hormone which you have injected just under the skin on a woman's arm. It can stay in place for three to five years. The implant gives off a steady supply of the hormone progestin, which prevents pregnancy.
It works by making the mucus around the cervix thicker so the sperm can't get through. And depending on the hormone dose, it can also stop the ovaries producing an egg. Implants are sold under the brand names Implanon, Norplant and Jadelle.
Vasectomy
Sterilisation for men. The tubes that carry sperm are blocked. You still ejaculate normally, but in the semen there aren't any sperm to fertilise an egg. This is a permanent method of contraception -- you can't get a woman pregnant any more.
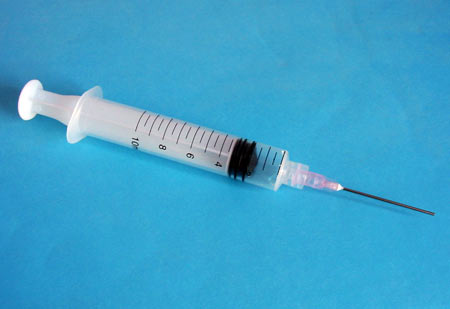
Combined shot
An injection of two different hormones, estrogen and progestin. Women have to have this injection every month. It stops your ovaries releasing an egg, so you can't get pregnant.
Hormonal IUD
A small cylinder about as long as a matchstick that is put inside the womb, or uterus (IUD stands for Intrauterine Device). A hormonal IUD is put in place by a doctor, and can stay there for up to five years.
It works by giving off a steady low dose of the hormone progestin. This makes the mucus around your cervix thicker so the sperm can't get through and can also stop your ovaries producing an egg. Hormonal IUDs are sold under the brand name Mirena.
Female sterilisation
The woman's fallopian tubes are blocked. These are the tubes that carry the eggs from the ovaries to the womb, or uterus. This is a permanent method of contraception – you don't produce any eggs any more, so you can't get pregnant.
Copper IUD
A little anchor-shaped plastic that is put inside the womb or uterus (IUD stands for intrauterine device). It's wrapped in a coil of copper wire -- which is why it's also sometimes called the 'coil'.
An IUD is put in place by a doctor, and can stay there for up to five years. Strangely enough, it isn't actually known exactly how the copper IUD works -- but it does work!
You can also have an IUD fitted as an emergency contraceptive, up to five days after you've had unprotected sex -- for example if a condom has torn or you've missed a pill.
This is the most popular contraception method in the world, mainly because millions of women in China use it.
© www.lovematters.info is a journalistic website about love, sex, relationships and everything in between.
Breastfeeding
If you're breastfeeding a baby you don't produce any eggs, so you can't get pregnant. But it only works for the first six months after the baby is born. And the baby has to be drinking enough milk, and not having any feeds replaced by formula milk or solids. And you have to breastfeed at least every four hours during the day and every six hours at night.
So breastfeeding works -- but you don't know exactly when you're going to become fertile again.
One-hormone shot
An injection of just one hormone, progestin, for women. You only have this injection every three months. It works by making the mucus around your cervix thicker so the sperm can't get through. It can also stop your ovaries producing an egg.

The pill
A pill women take once a day. It contains a combination of two hormones, estrogen and progestin (its full name is 'combined oral contraceptive pill'). The hormones stop you producing an egg, so you can't get pregnant.
You take the pill for three weeks, then take a one-week break, when you have a period. But usually the pills come in special 28-day packs, and in the break you keep on taking pills with no hormones in them. That way it's easier to remember.
The mini-pill
The 'mini-pill' is like the pill but only uses one hormone, progestin, instead of two. That's why it's properly called the progestin-only pill -- POP.
It works by making the mucus around your cervix thicker so the sperm can't get through. And depending on the hormone dose, it can stop your ovaries producing an egg. You take it in the same way as the 'ordinary' combined pill.
The patch
A small patch like a plaster, which women stick on the skin. It gives off a steady supply of the hormones estrogen and progestin, which pass through your skin into your bloodstream.
The hormones stop you producing an egg, so you can't get pregnant. You change the patch once a week for three weeks, then take a one-week break. The patch is sold under the brand names Ortho Evra or Evra.
Vaginal ring
A plastic ring you keep inside your vagina. It gives off a steady supply of the hormones estrogen and progestin. The hormones stop you producing an egg, so you can't get pregnant. The ring is about five centimetres across and made of flexible plastic.
You put it in place at the top of your vagina yourself, and keep it up for three weeks at a time. You can keep it in during sex. It's sold under the brand name NuvaRing.

Cervical cap
A rubber or plastic cap that fits over the cervix -- the neck of the womb, right at the top of the vagina. The cap blocks sperm from getting into the womb.
You have to be examined by a doctor to get the right size to fit your cervix. After that, you put the cap in yourself before you have sex. You can keep it in for 48 hours afterwards. For it to work properly, you have to use it with a spermicide -- a cream or pessary that kills sperm in your vagina.
If you've already given birth, you're more likely to get pregnant using this method. So for you it comes lower down this list, in the 'higher risk' category!
Saheli
Saheli is actually the brand name for a drug called ormeloxifene, or centchroman. Unlike the pill, or mini-pill, it doesn't contain hormones. It works by blocking the hormone estrogen. This means that when you produce an egg, the lining of the womb isn't ready to receive it.
For the first four months, you have to take the pill twice a week, and it's wise to use another birth control method as a back-up. After that you take it just once a week. Saheli is mainly used in India.
Condom
A rubber sheath that fits over the penis and stops sperm from getting into the vagina. It's like a very thin and stretchy tube-shaped bag, with a teat at the closed end to collect the sperm.
The condom comes rolled up in a flat foil package, which you tear to open. To put the condom on, you pinch the teat at the end to keep air out, then roll the condom down over the penis. You have to use a new condom each time you have intercourse.
Condoms are one of the most widely-used birth control methods. They also protect against a lot of sexually transmitted diseases, including HIV/AIDS.
Diaphragm
A soft rubber dome that fits over the cervix -- the neck of the womb, right at the top of the vagina. The diaphragm blocks sperm from getting into the womb.
You have to be examined by a doctor to get the right size to fit your cervix. After that, you put the diaphragm in yourself before you have sex.
You can keep the diaphragm in for 24 hours afterwards. For it to work properly, you have to use it with a spermicide -- a cream or pessary that kills sperm in your vagina.
Sponge
A sponge containing spermicide which you put in your vagina, right up inside over the cervix, the neck of the womb. It stops sperm from getting into the womb. At the same time the spermicide kills the sperm.
You have to use a new sponge each time you have intercourse. Sponges are sold under the brand names Pharmatex, Protectaid and Today.
If you've already given birth, you're more likely to get pregnant using this method. So for you it comes lower down this list, in the 'higher risk' category!

Female condom
A thin tube-shaped bag made of plastic or rubber which you put inside your vagina. It has a rubber ring at the closed end which fits up inside your vagina, and a larger one at the open end, which stays on the outside against your vulva. When you have intercourse, the penis goes inside the condom. You have to use a new one each time you have intercourse.
The condom keeps sperm out of your vagina to stop you getting pregnant. Female condoms also protect against a lot of sexually transmitted diseases.
Natural family planning methods
Methods where you avoid having sex when you are most fertile. This is around the time of ovulation, when your ovaries produce an egg. You don't get pregnant because you only have sex when there's no egg ready to be fertilised.
There are two main ways to work out when you are ovulating: look at the calendar, or look at your body for symptoms.
With a calendar-based method, you count the days between your periods. In the week before your period and the week after it starts you're least fertile. In the two weeks after that, you're most fertile. There are different ways to keep track of the days, ranging from counting beads to receiving text messages.
With a symptoms-based method, apart from being aware of the days between your periods, you also check your body for signs you are ovulating. You can do this by regularly taking your temperature, or checking look and feel of the mucus coming out of your vagina.
Withdrawal
The man pulls his penis out of the vagina before he ejaculates. No sperm gets in the vagina, so you don't get pregnant.
Withdrawal relies on the man getting the timing right. Especially for teenagers, it can be easy to make a mistake, and not pull the penis out in time.
Spermicide
Spermicides are chemicals that kill sperm in the vagina. They come as creams, films, foams, gels, or suppositories, which you insert deep inside your vagina.
They work by stopping the sperm from moving, so they can't swim up through the cervix to fertilise an egg. Spermicides don't work very well on their own. They're usually used to back up another birth control method, like a cap, diaphragm or condom.
These ways don't fit in the 'low risk to high risk' list because it's hard to compare them by working out their failure rate.
Abstinence
You don't have sex. Or at least not vaginal intercourse. So you don't get pregnant. Of course, you might opt for abstinence not just to avoid getting pregnant, but also because of your moral beliefs. Or simply because you don't feel ready for sex.
Abstinence obviously has a better 'perfect use' rating than all the birth control methods above -- its failure rate is zero! But the 'typical use' failure rate is higher.
People who don't mean to have sex sometimes get carried away and end up doing it after all. And because they're not planning on having sex, they sometimes end up not using any birth control whatsoever.
So it's been estimated that in reality the failure rate is about the same as for condoms -- in the 'medium risk' category.
Outercourse
'Outercourse' means making love, but avoiding vaginal intercourse. So you don't get pregnant. This is a slightly different take on not having intercourse compared to abstinence. The idea is you enjoy every kind of lovemaking there is, but keep the penis out of the vagina.
Again, the failure rate isn't zero, because in practice sometimes people get carried away and end up having vaginal intercourse, even though they didn't intend to.
And there's also a small risk of getting pregnant during lovemaking even without having intercourse -- for example, if you get sperm on your fingers and then put them in the vagina.
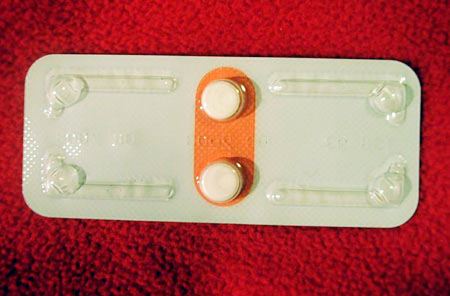
Emergency contraception (the 'morning after pill')
This is a pill you take after you've had unprotected sex to stop you getting pregnant. You can take it if a condom tears or you've missed a pill, for example, or if you get carried away and have sex without using birth control at all.
Emergency contraceptive pills give you a high dose of the hormones in normal contraceptive pills -- either progestin on its own or combined with estrogen. The emergency pill can stop you getting pregnant -- if you're already pregnant, it won't work, and it won't harm the baby either. It doesn't cause an abortion.
'Morning-after pill' isn't a very accurate name -- you have to take it within 72 hours of having sex. With the pill containing two hormones, this can be up to five days. It's not guaranteed to work. The sooner you take it, though, the better chance it has of working. This pill can make you feel unwell.
Emergency contraceptives don't fit on the list of methods in the previous pages, because they're not meant to be used as a regular form of birth control -- only in emergencies. That means you can't compare their failure rate over consistent use.