'We urge the government to have discussions with private labs on the actual cost of running a test.'
Aneesh Phadnis reports.

Diagnostic laboratories say the capping of RT-PCR rates by state governments will make their business unviable and could lead to a reduction in their testing capacities.
The reactions came in the wake of the Maharashtra government's announcement to cap the minimum rate of RT-PCR test at Rs 500 and rapid antigen test at Rs 150.
"It is an extremely challenging situation for private labs," says Sushant Kinra, chief operating officer, Suburban Diagnostics, which runs 200 centres across 16 cities in Western India.
"Such low level of price capping makes routine operations of a lab strenuous," Kinra adds. "We urge the government to have discussions with the private labs on the actual cost of running a test and arrive at an agreeable disposition."
A similar sentiment was echoed by Ameera Shah, secretary of the industry body NATHEALTH that called upon the government to hold consultations with laboratories before fixing prices.

"Private diagnostic labs have played a pivotal role in expanding testing and strengthened their capacities to meet the periodic surge in cases. For the certified labs this (price capping) can lead to reduction of testing capacity as most of them will not be able to conduct tests at these prices, in contrast to what the country needs at this time," says Shah.
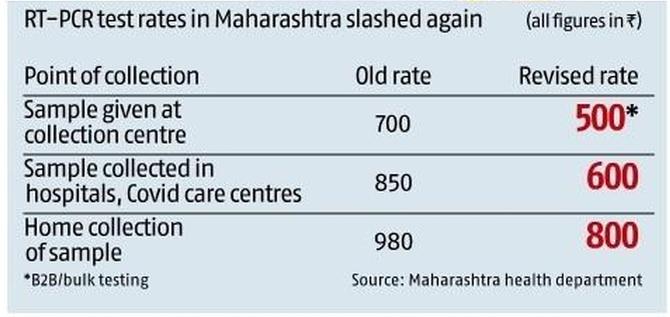
According to the revised rates announced by the Maharashtra health department, laboratories can charge Rs 500-Rs 800 for RT-PCR tests.
The Rs 500 fee applies to B2B clients and bulk testing. Samples collected from a collection centre can be charged Rs 500 and those from hospitals or COVID-19 centres would be priced at Rs 600.
Home collection of samples would cost Rs 800 according to the new order. Rapid antigen tests will cost Rs 150-Rs 300.
This was the fourth price revision in test rates in Maharashtra and came in the backdrop of a surge in cases.
Delayed testing owing to a lack of discipline among patients has increased the burden on hospitals.
The Maharashtra government wants to increase testing and contact tracing to reduce caseload.
In January, Uttarakhand and Haryana slashed the minimum price of RT-PCR tests to Rs 500.
A month earlier, rates were capped in Uttar Pradesh, Karnataka and Telangana.
The Maharashtra government justified the price reduction citing easy availability of inputs required for testing.
The order said that reagents, viral transport medium kits, personal protective equipment gear and N95 masks are now available at reasonable rates.
But lab owners differ. "It is challenging to work at costs dictated by the state government. HR costs and biomedical disposal costs are more worrying than the actual reagent costs, says Dr A Velumani, founder and chairman of Thyrocare.
"However, if floor efficiency is good and overheads are controlled it is possible to work even at these rates in the larger interests of state and society," Dr Velumani adds.
"When the government is capping prices," an industry executive points out, "it is only looking at the rates of chemicals or reagents. But these only account for 25-30 per cent of the expenses for a laboratory."
"A major item is servicing cost," the executive adds." Today, when we ask a phlebotomist to collect a COVID-19 sample from home we need to pay a decent allowance. Plus there are transport and PPE gear costs."
"If you add up all these then it would become unviable to carry out the tests with reduced charges," the executive adds.
"For smaller labs, who have capacity to do only 200-300 tests a day it is harder because they don't get reagents at the same rates as the larger labs," the executive explains.
Dr Lal PathLabs, however, does not see much impact of Maharashtra's latest price capping order.
"West India's contribution to our business is not significant," says Om Manchanda, managing director, Dr Lal PathLabs. "Recovery of non-Covid business to 2019 level and improved efficiencies has enabled us to absorb rising costs and maintain profitability."
Feature Presentation: Rajesh Alva/Rediff.com











