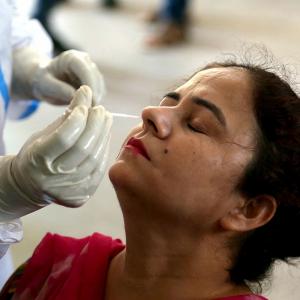
The presence of antibodies indicates previous exposure to the SARS-CoV-2 virus but may not always translate into protection against the disease, say scientists, citing imponderables such as what kind of antibodies, how many and how long they last.
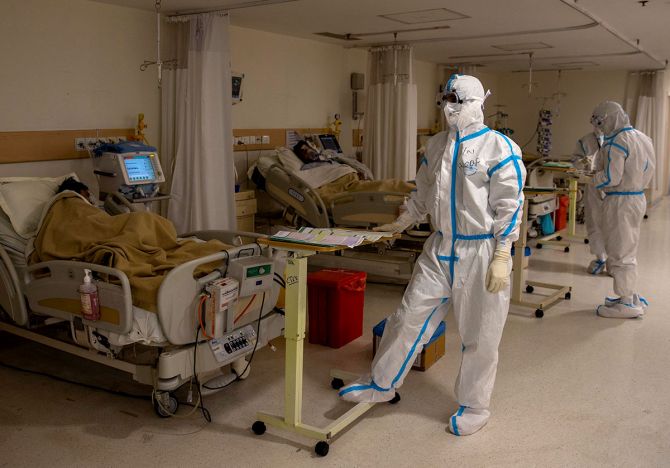
As worries over India's COVID-19 spike mount -- the country added 75,809 cases on Tuesday to take its tally to 42,80,422 -- scientists are grappling with the pivotal issue of antibodies and trying to understand how they impact on the progression of the disease.
But the jury is still out there with several studies and hypotheses but no consensus yet. The only thing that can be said with any degree of uncertainty is that antibodies are a sign the person has already been infected with the novel coronavirus, the scientists said.
Immunologist Satyajit Rath said he would prefer to 'wait and see' where the evidence goes.
Antibody presence in itself tells us nothing about disease progression in individuals, said the scientist from New Delhi's National Institute of Immunology.
There are neutralising antibodies and also 'simple' antibodies. While nAbs produced against the novel coronavirus can block its entry into the host cell, other antibodies are also generated against many parts of the virus, added Vineeta Bal from Pune's Indian Institute of Science, Education and Research.
The 'simple' antibodies are an indication of host response to viral presence but are not that useful to stop further spread of the virus, Bal said.
"Simple presence of antibodies is a clear indication of previous exposure to SARS-CoV2 but does not necessarily guarantee protection from the disease in the absence of neutralising antibodies," the immunologist added.
"Presence of nAbs in sufficient concentrations and for longer period is the most likely indicator of protection of the individual from next exposure leading to illness i.e. COVID-19," she explained.
Bal also noted that there is no consensus on what levels of nAbs are 'protective' from the public health perspective or to ensure that plasma therapy is likely to be useful.
Different sero-survey tests have been conducted in India in the last few months with the aim of indicating the actual number of infected cases in the country.
A sero-survey involves testing the blood serum of a group of individuals for the presence of antibodies against that infection to know who has been infected in the past and has now recovered.
Surveys carried across metros suggest that COVID-19 cases are far more than actually reported.
According to Rath, one of the many problems in looking for easy patterns in the serological evidence is that not everyone is using the same antibody tests.
"In fact, all antibody tests in the market are not against the same viral protein target, and some investigators use only one target, others use more. And it is possible that tests differ in their sensitivity," Rath said.
The scientist also noted that most surveys are reporting people as just 'positive' or 'negative', and not analysing antibody levels present in the blood.
So far, the limited evidence available does indicate that these antibody tests seem to correlate with 'protective' antibody levels too. However, there is not much that can be said to individual people about their risk of reinfection or their level of protection.
Different studies, including one published recently in the Journal of Clinical Microbiology, have also suggested that people infected with COVID-19 develop neutralising antibodies that can protect them from reinfection.
However, reinfection cases reported recently from across the world have dented that optimism.
Shining more light on the issue, Bal said reinfection of an individual does not mean he or she becomes ill with COVID-19.
Even the presence of enough nAbs capable of neutralising a variant virus will not necessarily prevent infection, said Bal. However, in all probability, such a person with 'protective immunity' is likely to handle subsequent infections -- including what is currently reported as reinfection -- better and with less morbidity than otherwise.
"Reinfections should not be equated with disease due to repeat exposure to the same or related virus," she said, adding that the recent case of reinfection in the person in Hong Kong was discovered due to screening test rather than symptoms.
While it is not clearly known whether people who generate antibodies against SARS-CoV-2 are protected from reinfection, scientists also don't know how long those antibodies persist.
A study published in the NEJM journal on September 1 found that antibodies against the new coronavirus endure in the body for four months after infection, countering earlier evidence suggesting these important immune molecules disappear quickly.
The study measured the levels of SARS-CoV-2 antibodies in the blood of roughly 30,000 people, including more than 1,200 who had tested positive for the virus and recovered from COVID-19 in Iceland.
Around 90 per cent of the recovered people had antibodies against the virus.
"Based on the Iceland study, we know that antibodies generated by natural infection can last for four months, maybe longer," said Bal.
At the moment, there is no idea what percentage of previously exposed people will be susceptible to antibody mediated enhancement of the disease when re-exposed to a variant of SARS-CoV-2 or a related virus, she added.
ADE is a phenomenon in which the binding of a virus to antibodies enhances its entry into host cells followed by its replication. It is a general concern for the development of vaccines and antibody therapies.
Rath noted that the Iceland study seems to be quite thorough in many respects, and shows antibody persistence till about four months.
"Is this going to be the case everywhere? I have no guess to offer I am afraid. As far as disease progression in communities goes, the antibody evidence does tell us how much the virus has spread and in which locations-communities, although we need to do much more detailed and repeated sero-surveys to be able to learn anything more than 'it has spread quite a bit, or maybe a lot'," Rath said.